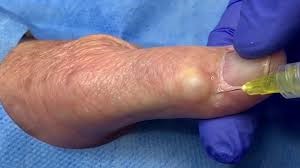
What is it…?
A myxoid cyst, or digital mucous cyst, is a small, noncancerous bump most often found near a joint at the end of your finger. It is a sac filled with fluid that appears on the finger, above the joint located next to the nail (the distal interphalangeal joint). The stalk of the mucous cyst is often connected to the DIP joint. Mucous cysts are firm and do not easily move under the skin. They may become painful, however, most mucous cyst are not. At times, the location and pressure from the cyst on the nailbed may cause a groove in the fingernail. Mucous cyst ganglions often will develop in middle age or older patients with wear and tear arthritis.
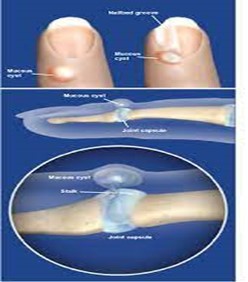
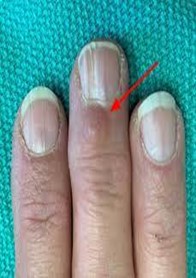
Who do myxoid cysts affect?
Myxoid cysts can affect anyone, but they’re most common in adults ages 40 and up. They affect people assigned female at birth three times as often as people assigned male at birth. Between 64% and 93% of people with osteoarthritis have myxoid cysts.
Associated symptoms…
- These cysts are most common near the nail on the index, middle or ring finger of your preferred (dominant) hand. They’re not as common on your toes. You’ll usually only have one cyst, but you may develop more than one.
- Myxoid cysts have a smooth, shiny surface. They’re usually skin-colored and look almost translucent (light can shine through). They range in size from 5 millimeters to 1 centimeter across, which is about the size of a pencil eraser. The round or oval bumps may be firm or filled with a jelly-like, sticky fluid. They typically don’t cause any pain. However, you may experience arthritis pain and stiffness in the nearby joint.
- Rarely, a myxoid cyst may grow under your nail or involve the root of the nail. This type of cyst can be painful. It can cause a groove to develop down the length of your nail. You may also see slight depressions or color changes. Your nail may split or you may lose your nail.
- If the cyst does rupture, it needs medical attention. At the base of the cyst is a stem connected to the joint, and when the cyst ruptures, it leaves a path directly into the joint that exposes it to possibility of deep infection inside the joint. In this case, I will prescribe antibiotics that should be applied directly onto the site of the rupture, and the finger should be wrapped in a dressing. It is likely that I will also prescribe oral antibiotics in addition. If the joint still develops an infection, the next step will be surgery.
Causes:
Researchers aren’t exactly sure what causes myxoid cysts. They appear to form when connective tissue weakens (degenerates). There are two variations:
- Osteoarthritis: Osteoarthritis and other degenerative diseases can cause the lining of your joints to grow excessively. This type of cyst looks like a ganglion cyst, which has a stalk that tracks back to the joint. Mucous Cyst is commonly related to osteoarthritis affecting the joint where the cyst develops. Though it is not known exactly how they develop, it is thought that the cysts are formed when connective tissue that connects the tendons in the finger, wears away. When is happens, is it thought that collagen from the degenerated connective tissue is left behind and begins to collect in pools which then form cysts.
- Focal mucinosis: This condition occurs when abnormal deposits of mucins (mucopolysaccharides) build up in the skin under your finger or toe. Mucins are part of your mucus. This type of cyst isn’t associated with joint degeneration.
My Examination:
I typically can diagnose a myxoid cyst with a physical exam. I will look at and feel the cyst. I will also ask you questions about the cyst, including:
- How fast has it been growing?
- Does it cause you any pain?
- Have you noticed any color changes?
- Have you had any recent trauma to the area?
An X-ray can show evidence of osteoarthritis. A biopsy can rule out other medical conditions.
Management and treatment:
Myxoid cysts may shrink or go away on their own. However, if they don’t, they’re usually not painful and don’t cause any other symptoms. Even when a cyst does disappear, it often comes back.
There aren’t many digital mucous cyst home treatment options. You can try firmly pressing on the cyst repeatedly for several weeks. Some studies say 39% of cysts may disappear using this method. But you shouldn’t try to drain or puncture the cyst yourself. This can cause an infection. Some people have tried applying a topical steroid to their cysts, but there’s no strong evidence that this method is effective.
If it is starting to cause you pain or affecting your quality of life, it may be time to make an appointment to have it evaluated professionally.
After the evaluation I will make my recommendations and then together we will determine the best treatment option for the patient.
- Repeated sterile draining: Your provider will use a sterile needle or knife blade to puncture and drain the cyst. They may need to repeat the procedure two to five times. Occasionally, a steroid compound may be injected into the cyst sac. This also has the potential for infection and a very high recurrence rate.

- Surgical removal is the most effective treatment for this cyst, with a higher than 90% success rate. During surgery, I will cut the cyst away. I will also scrape the involved joint and remove any bony outgrowths from the joint cartilage (osteophytes).
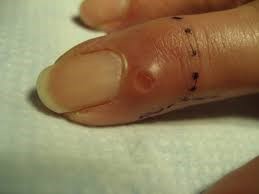
Outcomes and Postoperative Management:
If treated with surgery, you will have a soft dressing that covers the operative finger but leaves the tip exposed so you can monitor the circulation to your finger. You can expect your operative finger, and perhaps its neighbors, to be numb from the local anesthetic for about 24 hours. You will be seen in the office approximately 10 days after the procedure for a wound check and suture removal.
As I probably explained to you in the office, you can expect the joint to be uncomfortable for anywhere from 1 to 3 or so weeks and this should diminish significantly over that time. This does not mean you will not be able to use your hand, just that it will be sore. The joint will also be stiff for a few weeks as there will be swelling, and because I will have removed bone spurs from the joint.
Most people do not require therapy to help recover from a mucous cyst excision. On the other hand, I will offer it if it seems that your recovery is not progressing quickly.
If you feel as if you or any of your family and friends could have any of the symptoms provided here, medical care is available. Dr Ayisha Livingstone is a Fellowship Trained and Board-Certified Orthopedic Hand Surgeon in Fort Lauderdale, FL. To learn more or book a consultation, click here.

